Rudy Ramos, Mouser Electronics
Often when we are unwell we can ‘feel’ the symptoms but, in many cases, we misinterpret the signals due to lack of training and even anxieties that mask the true issue. In this article, we will look at how technology is being used to monitor and assess as well as assist in the healing process.
The average age of the world’s population is increasing, people are living longer and there is a general reduction in the birth rate. Caring for the elderly is requiring more resources and with fewer young people to step into these roles, medical professionals are exploring the role technology can play in bridging this gap.
There are several trends in the technology arena that are making this possible. The IoT is delivering a highly connected world, semiconductors are getting smaller, smarter and more efficient and artificial intelligence has developed to a point where it identifies symptoms at least as well as a human. Bringing this together gives a very exciting outlook for the future of technology in healthcare.
Many people these days have a wearable biometric monitor that measures pulse rate and other vital signs. These small devices are worn unobtrusively on the wrist yet, in future, it may become possible to weave this technology directly into the fabric of clothing making it even less obtrusive.
While these smart fabrics could improve monitoring but there are other, more interesting, applications. There is currently significant research into how smart fabrics can not only monitor but also play a role in administering medication – with some early examples already in place.
Pressure on recovery
As we heal, the affected area often swells and, to an extent, this can be a good thing as it is a natural part of the healing process. However, monitoring is essential as too much swelling can be an indication of an issue or even an unexpected infection. If the patient is bed-bound while healing then pressure sores may develop that impact the healing process. Therefore it is essential to monitor not only the wound but also the patient’s movement.
One technology that is in development is silicone-coated, electrically conductive yarn that can be woven into clothing or even hospital bed sheets. The yarn has the ability to monitor movement and moisture, alerting medical staff if the patient needs care. Taking this one step further, the same technology could automatically move a powered bed, reducing the need for medical staff to perform mundane tasks.
The same technology could also be incorporated into bandages to monitor how quickly swelling reduces as part of the healing process or even to send an alert if the bandage has been applied too tightly.
Measuring blood pressure is very common as part of many health checks. The basic principle is that a cuff is placed around the arm and inflated until the blood stops. Originally performed manually with the aid of a stethoscope, semi-automatic blood pressure monitors are now relatively common, even for home use. It would be relatively simple to integrate the same technology into the clothing worn by athletes to allow continuous monitoring during exertion.
There are other applications for pressure monitoring in the medical world. A patient may have an issue with the way they walk, either due to an injury or an issue such as peripheral neuropathy, or some other cause. By placing pressure monitors in the insoles of shoes the pressure exerted by each foot while walking can be recorded and sent to a smart device for analysis or transmission to a doctor. One example of a system that does this is shown in Figure 1.
 Figure 1: The Orpyx system uses pressure sensors embedded in an insole and wirelessly connected to a smartphone (Source: www.orpyx.com)
Figure 1: The Orpyx system uses pressure sensors embedded in an insole and wirelessly connected to a smartphone (Source: www.orpyx.com)
Smart fabrics can also measure skin distortion and fabrics capable of this are now in development. Another benefit of using dressings and bandages for monitoring is that long-term trends can be recorded and analyzed which shows progress of the current condition and may also allow early diagnosis of other conditions.
Nanotechnology makes plasters smarter
Nanotechnology has allowed hydration to be assessed through monitoring the electrical characteristics of the patient’s skin. Currently this involves embedding tiny wires into stretchable fabrics but this could also be implemented in clothing fabrics in future. In either case the tiny electrodes are able to communicate the hydration levels in real time.
Impedance spectroscopy is a technique whereby the capacitance and resistance of cells is measured as they decay by passing a small electrical current through the patient’s cells. Embedding this technology into smart dressings allows issues such as bedsores to be identified and treated before they become visible to the naked eye.
Combining electronic technology with traditional medicine brings further opportunities, such as giving the ability to deliver medication in direct response to the monitoring of a condition. This would make the administration of the medication far more effective – and efficient. An early demonstration of the technique has been shown by researchers from a combination of the University of Nebraska-Lincoln, Harvard Medical School and MIT.
Described as the first example of a bandage that can deliver dose-dependent drugs (including antibiotics and pain-killers) the solution uses medicines embedded within a gel which is used to cover wires embedded within the dressing / bandage. An intelligent system based on a microcontroller delivers a current through the wires that heats the gel and disperses the drug to the area where treatment is required.
Initial trials have been positive and further advances being considered include adding the capability to measure pH levels and glucose, thereby giving a fully automated process.
Taking this even further, targeted treatments are now being researched whereby nanoparticles can be used to deliver treatments right down to the cellular level. This is good for patients as they no longer have to metabolize the drug and have it travel around their entire body, so lower doses can be used directed at the specific area of need. The treatment is also expected to be more effective this way. Health providers will also benefit as the combination of lower doses and a more effective delivery will reduce their costs.
The benefits of being connected
Combining the IoT with recent developments in Artificial Intelligence (AI) allows large-scale data to be analyzed for trends. When applied to medical data gathered from a large sample of patients through the IoMT, this analysis could provide better insights into conditions and be used to improve future treatments.
In order for this to be effective a holistic approach will be required with greater use of compatible technology by healthcare providers and also common data sets that allow data to be easily combined.
The role of MEMS technology
With the need for positional awareness in many aspects of modern life, including drones/UAVs, smartphones and modern vehicles, the ability for MEMS technology to deliver multi-axis sensing is becoming very important. MEMS is also behind the microphones that are used in modern hearing aids, allowing their performance to improve while they become smaller at the same time.
Other uses for MEMS in medical applications are being researched. One possibly application is in eye medicine to check for early signs of glaucoma. Changes in the intra-ocular pressure (IOP) in the eye are a key indicator of this and, by mounting a MEMS microphone onto a disposable contact lens changes in IOP that indicate a change in the shape of the cornea can be detected, giving early warning of glaucoma.
The Swiss company, Sensimed, have launched a MEMS-based IOP sensing system that includes in-built wireless communication via NFC. Figure 2 shows how the system comprises three elements: the disposable contact lens with an embedded sensor and transducer (1), a separate antenna that is worn around the eye (2), and the data recorder (4), connected by a thin wire (3).
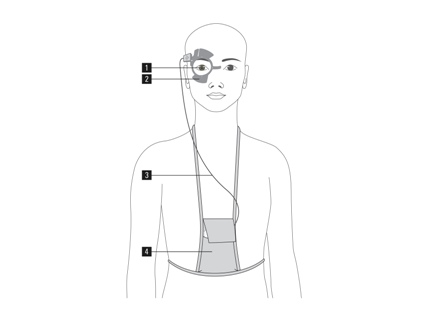 Figure 2: Sensimed’s IOP sensor in integrated into a disposable contact lens, which is powered and connected using NFC (Source: www.sensimed.ch)
Figure 2: Sensimed’s IOP sensor in integrated into a disposable contact lens, which is powered and connected using NFC (Source: www.sensimed.ch)
NFC is an ideal protocol for many medical applications as the sensor requires no dedicated power source, instead it is energized by the RF energy from the reading device, allowing it to make a measurement and transmit the data. As the battery is often the largest part of any system, its removal brings many more opportunities for ultra-small sensors to be embedded in areas where it was not previously possible, such as smart fabrics.
Summary
Technologies such as smart fabrics and nanotechnology, along with advanced low power electronics and smart connectivity have the potential to revolutionize medicine. While much of this exists at the research level today, practical applications are starting to emerge and it is expected that many more will become mainstream soon. The IoMT and the associated devices will soon change the doctor-patient relationship and make high-quality medical care more accessible for all.






